Introduction
Cells are the basic living units of the human body. Every tissue, organ, and biological system depends on the coordinated work of cells. Although cells are microscopic, their activities shape everything from growth and energy production to immunity, healing, and brain function. To understand health, it is therefore essential to understand cells.
The human body contains trillions of cells, but these cells are not all the same. Muscle cells contract, neurons transmit signals, immune cells defend against infection, and epithelial cells form protective barriers. Each cell type has specialized functions, yet all cells share core features: they obtain energy, maintain internal balance, sense their environment, and communicate with other cells.
Health depends on the ability of cells to function properly and to respond appropriately to changing conditions. When cells are damaged, deprived of nutrients, exposed to toxins, infected by microbes, or affected by abnormal signaling, tissues may no longer work as they should. In this sense, many diseases can be understood as disorders of cellular function, communication, or repair.
Studying cells provides a bridge between molecular biology and whole-body medicine. It helps explain how health is maintained, how disease begins, and why different organs respond differently to stress or injury.
Concept
A cell is the smallest unit of life capable of carrying out essential biological processes. Each cell is surrounded by a membrane that separates it from the external environment and helps regulate what enters and leaves. Inside the cell are structures known as organelles, each with a specialized role.
Some of the most important cell components include:
Cell membrane
This outer boundary helps protect the cell and controls the movement of substances such as ions, nutrients, and signaling molecules.
Nucleus
In most human cells, the nucleus contains DNA, which stores genetic information and helps regulate cell activity.
Mitochondria
These organelles generate much of the cell’s usable energy in the form of ATP, making them essential for metabolism and survival.
Endoplasmic reticulum and Golgi apparatus
These structures help synthesize, modify, and transport proteins and lipids.
Cytoskeleton
This internal framework gives the cell shape and supports movement, transport, and organization.
Cells are highly dynamic rather than static. They constantly sense their surroundings, exchange materials, repair damage, divide when needed, and sometimes undergo programmed cell death to protect the organism as a whole. In healthy tissues, these processes are tightly regulated.
Cells therefore do more than simply exist within organs. They are active participants in maintaining physiological stability, adapting to change, and preserving health across the entire body.
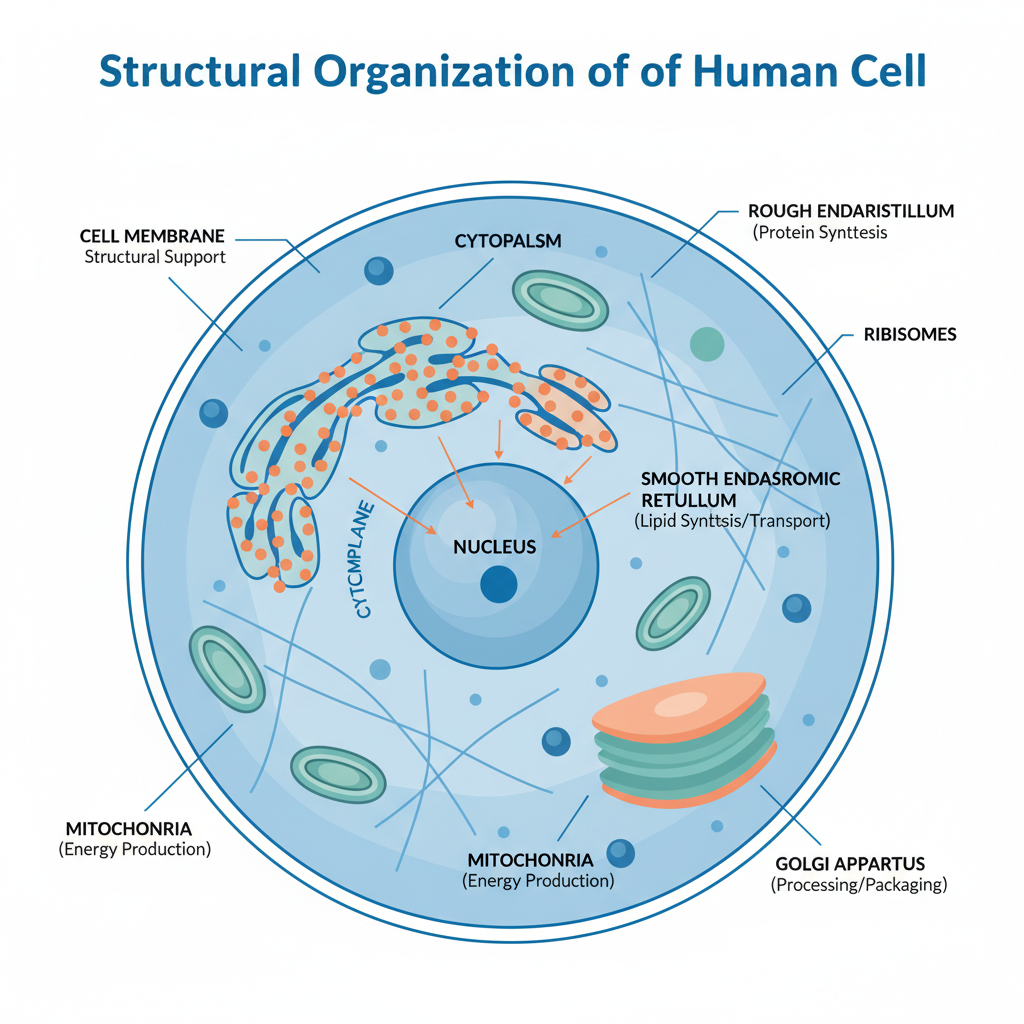
Figure 1. Structural organization of a human cell and its major functional components. Representative schematic of a human eukaryotic cell illustrating the major organelles, including the plasma membrane, cytoplasm, nucleus, rough and smooth endoplasmic reticulum, ribosomes, mitochondria, and Golgi apparatus. These structures coordinate essential cellular functions such as compartmentalization, gene regulation, protein and lipid synthesis, energy production, and intracellular processing and transport.
A typical human cell contains specialized structures that support essential biological functions. The cell membrane regulates exchange with the environment, the nucleus stores genetic information, mitochondria generate energy, and intracellular organelles coordinate protein synthesis, transport, and cellular organization. Together, these components enable cells to maintain homeostasis and respond to internal and external signals.
Mechanism
Cellular health depends on several core processes. One of the most important is metabolism, the set of chemical reactions that allows cells to convert nutrients into energy and building materials. Glucose, fatty acids, amino acids, oxygen, and micronutrients all contribute to cellular activity. If energy production fails, the cell cannot maintain membrane transport, signaling, or repair.
Another key process is gene expression. Although nearly all cells contain the same DNA, different cell types activate different sets of genes. This allows a liver cell, neuron, and immune cell to perform distinct functions. Gene expression is influenced by developmental programming, hormones, nutrients, stress signals, and environmental conditions.
Cells must also regulate signal transduction, the process by which external messages are converted into internal responses. Signals may come from hormones, neurotransmitters, growth factors, cytokines, or neighboring cells. These molecules bind to receptors on the cell surface or inside the cell, activating pathways that alter metabolism, movement, gene expression, or survival.
Examples of cellular responses include:
– increasing glucose uptake in response to insulin
– activating immune genes in response to infection
– initiating repair pathways after injury
– dividing in response to growth signals
– undergoing apoptosis when damage is too severe
The body also relies on cell cycle control. Some cells divide frequently, while others divide rarely. Division must be carefully regulated so that tissues can grow and repair without uncontrolled proliferation. When cell cycle regulation is lost, abnormal growth and cancer may develop.
Cells are further protected by quality-control systems such as antioxidant defenses, DNA repair, protein-folding mechanisms, and waste removal pathways including autophagy. These systems help preserve function under stress. When stress becomes prolonged or overwhelming, however, these protective mechanisms may fail.
Thus, cellular function depends on a balance between energy supply, signaling accuracy, repair capacity, and environmental adaptation.
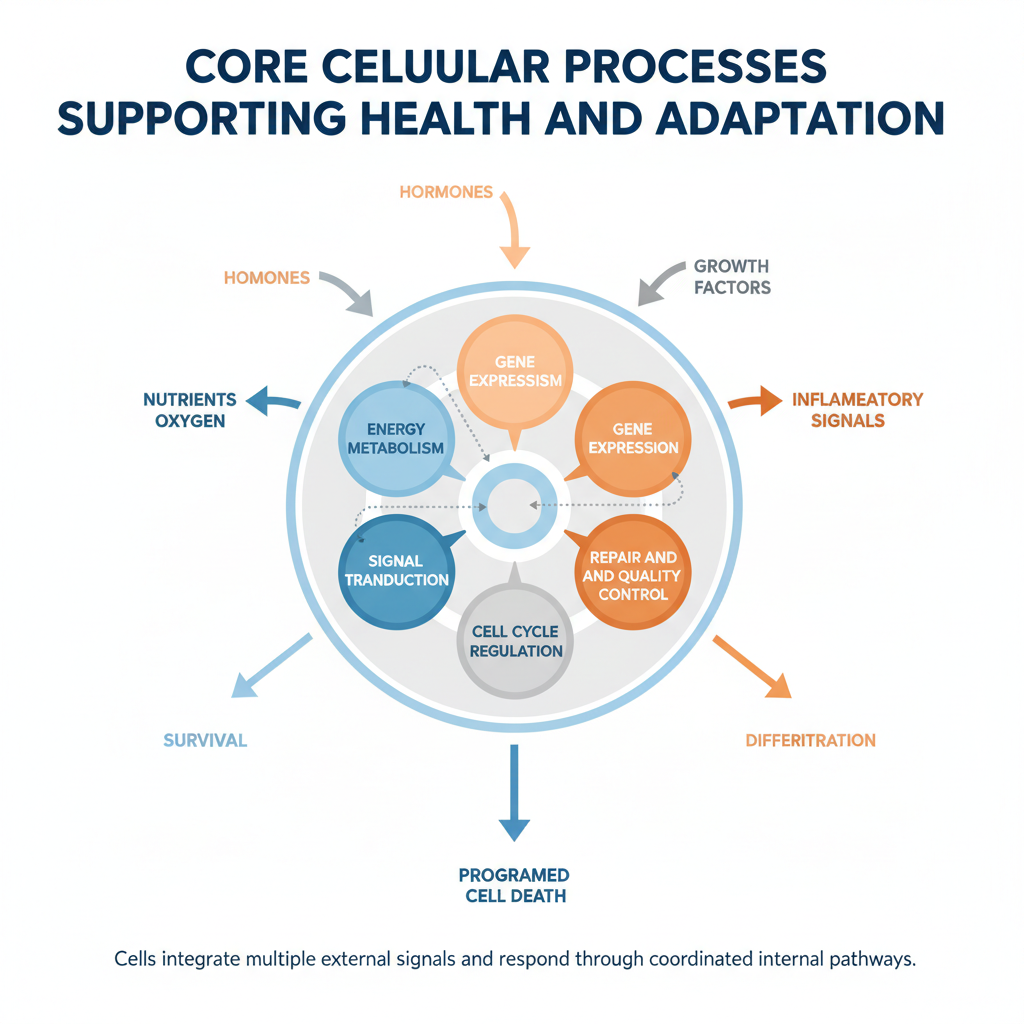
Figure 2. Core cellular processes supporting health and adaptation. Cells integrate extracellular signals, including nutrients, oxygen, hormones, growth factors, and inflammatory mediators, through interconnected intracellular pathways. These inputs regulate fundamental processes such as signal transduction, energy metabolism, gene expression, cell cycle control, and cellular repair and quality control, which together determine cellular fate and adaptive responses, including survival, differentiation, and programmed cell death.
Cellular health depends on coordinated regulation of energy metabolism, gene expression, signal transduction, repair pathways, and cell cycle control. External signals such as nutrients, hormones, stress mediators, and inflammatory factors are integrated through intracellular pathways that influence survival, adaptation, proliferation, or programmed cell death.
Systems Perspective
Although a single cell can perform many functions, human health depends on communication among vast numbers of cells organized into tissues and organs. Cells rarely act alone. Instead, they form networks.
In the nervous system, neurons communicate through electrical impulses and neurotransmitters, allowing rapid control of sensation, movement, and cognition. In the endocrine system, specialized cells release hormones into the bloodstream, coordinating metabolism, growth, reproduction, and stress responses across distant organs. In the immune system, cells detect pathogens and tissue injury, then communicate through cytokines and direct cell-to-cell interactions. In the circulatory system, blood cells and endothelial cells help transport oxygen, nutrients, immune mediators, and waste products.
This intercellular communication is essential for homeostasis. For example:
– pancreatic beta cells sense blood glucose and release insulin
– muscle and liver cells respond to insulin by changing glucose metabolism
– immune cells detect infection and recruit additional defense cells
– skin and epithelial cells form barriers while signaling tissue damage when injured
– stem cells respond to repair signals during regeneration
A problem in one cell population can therefore affect many others. Mitochondrial dysfunction in muscle may reduce energy balance. Abnormal signaling in fat tissue may promote systemic inflammation. Endothelial injury in blood vessels may alter circulation and increase cardiovascular risk. Neuroinflammation may affect mood, cognition, and behavior.
A systems view reminds us that cellular health is not only a microscopic issue. Cellular events accumulate into tissue responses, organ performance, and whole-body health outcomes.
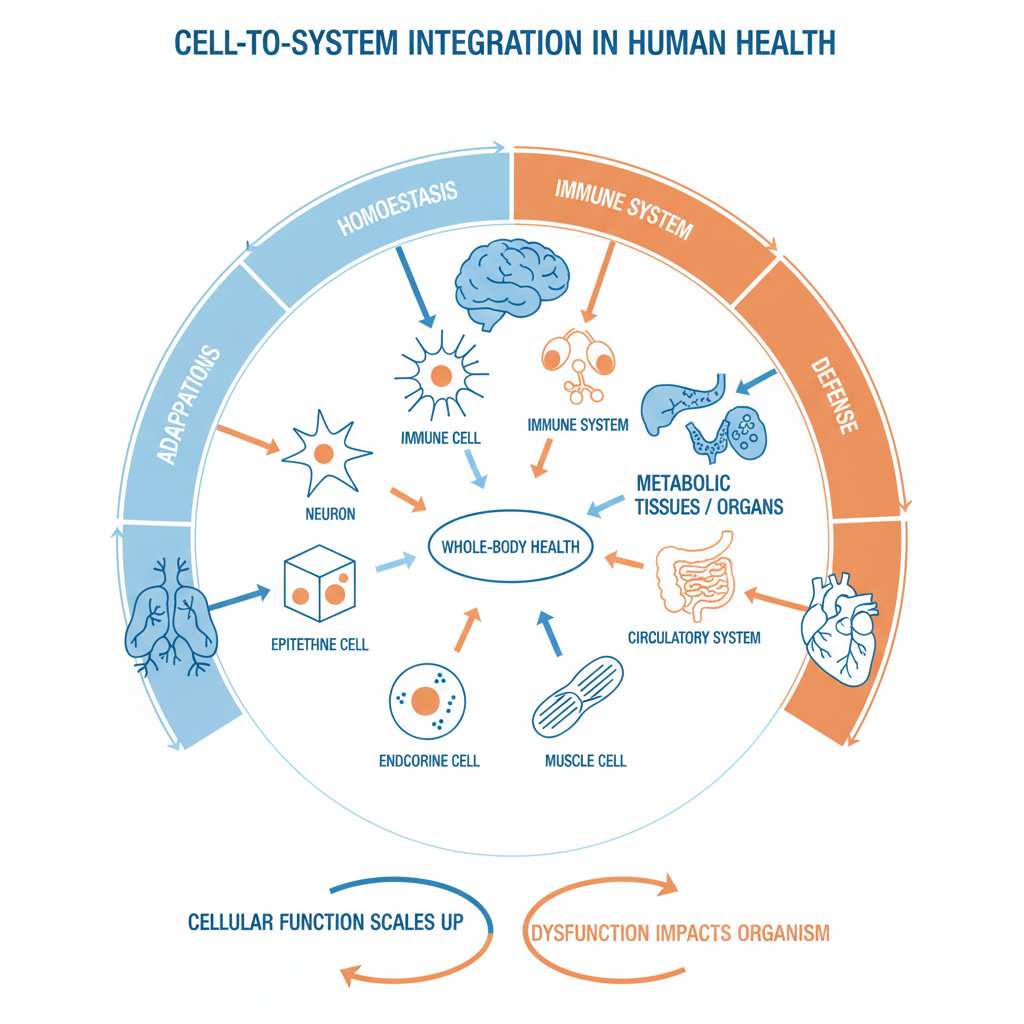
Figure 3. Cell-to-system integration in human health. This schematic depicts the multiscale organization of human physiology, showing how cellular functions are integrated into tissue, organ, and whole-body systems. Specialized cell types, including neurons, epithelial cells, immune cells, endocrine cells, and muscle cells, interact with higher-order physiological systems such as the immune system, metabolic tissues and organs, and the circulatory system. These interconnected networks collectively support essential organismal functions, including homeostasis, adaptation, and defense, thereby contributing to whole-body health. The diagram also emphasizes that cellular function scales upward to influence systemic physiology, whereas cellular dysfunction can propagate across levels of biological organization and adversely affect the organism as a whole.
Cells function within organized networks that form tissues, organs, and physiological systems. Signals exchanged among immune cells, neurons, endocrine cells, vascular cells, and metabolic tissues coordinate homeostasis, adaptation, and repair. Disruption of cellular communication in one tissue can propagate across systems and contribute to broader disease processes.
Health Connections
Many common diseases can be understood at the cellular level. This does not mean that all disease is caused by a single cell defect, but rather that illness often develops when cellular processes are persistently disrupted.
Examples include:
Metabolic disease
In insulin resistance and type 2 diabetes, cells do not respond normally to insulin signaling, leading to impaired glucose uptake and altered energy regulation.
Cardiovascular disease
Damage to endothelial cells, abnormal lipid handling, oxidative stress, and chronic inflammation contribute to vascular dysfunction and plaque formation.
Cancer
Cancer involves dysregulated cell growth, failure of normal death pathways, altered gene expression, and changes in communication between cells and their environment.
Neurodegenerative disease
Neurons are highly dependent on energy production, protein quality control, and synaptic communication. Failures in these systems can contribute to progressive brain disorders.
Infectious disease
Viruses, bacteria, and other pathogens can invade cells, disrupt normal function, trigger inflammation, and damage tissues.
Aging
Over time, cells accumulate molecular damage, reduced repair capacity, altered signaling, and changes in mitochondrial function. These shifts can contribute to declining resilience and increased disease risk.
Lifestyle factors strongly influence cellular health. Balanced nutrition provides substrates for metabolism and repair. Physical activity improves mitochondrial function and signaling sensitivity. Sleep supports restoration and immune regulation. Chronic stress, smoking, pollution, and poor diet can increase oxidative stress, inflammation, and cellular dysfunction.
Understanding cells therefore helps explain why prevention matters. Healthy daily habits support cellular resilience long before disease becomes clinically visible.
Integrative Perspective
Across many medical traditions, health has often been linked to vitality, balance, and proper internal regulation. Modern cell biology provides a detailed scientific framework for these ideas. Cells must continuously maintain balance in energy use, signaling, repair, and interaction with the environment. When regulation is stable, tissues function well. When stress overwhelms adaptation, dysfunction may spread from cells to organs and then to the whole body.
This perspective also helps bridge reductionist and holistic views of medicine. Cells are small, but their behavior reflects the integrated influence of genes, nutrients, hormones, microbial exposure, physical activity, psychological stress, and social conditions. Cellular health is therefore both a molecular and a systemic phenomenon.
For learners, this is an important insight: to study cells is not to move away from real-life health, but to understand its foundations more clearly.
Key Takeaways
– Cells are the basic living units that make up all tissues and organs.
– Major cell structures such as the membrane, nucleus, mitochondria, and cytoskeleton support essential biological functions.
– Cellular health depends on energy metabolism, gene expression, signaling, repair, and regulated cell division.
– Cells communicate through hormones, neurotransmitters, cytokines, and direct contact.
– Many diseases involve disrupted cellular function, communication, or adaptation.
– Healthy lifestyle factors help maintain cellular resilience and long-term health.
-95x98.png)